
Arizona Medicare plans include Original Medicare Parts A and B, Part C (Medicare Advantage), Part D (prescription drug coverage), and Medicare Supplement (Medigap) coverage. To make the most of your coverage, it is essential to understand your options to make an informed decision when selecting your health plan.
Medicare is designed to provide and reduce the cost of healthcare in the United States. You are eligible for Medicare in Arizona if you meet one of three criteria:
If you meet one of the above criteria, you qualify for Medicare in Arizona and can apply. Continue reading to learn about Medicare plans in Arizona, essential enrollment periods, and how to find the health coverage that fits your health and budget.
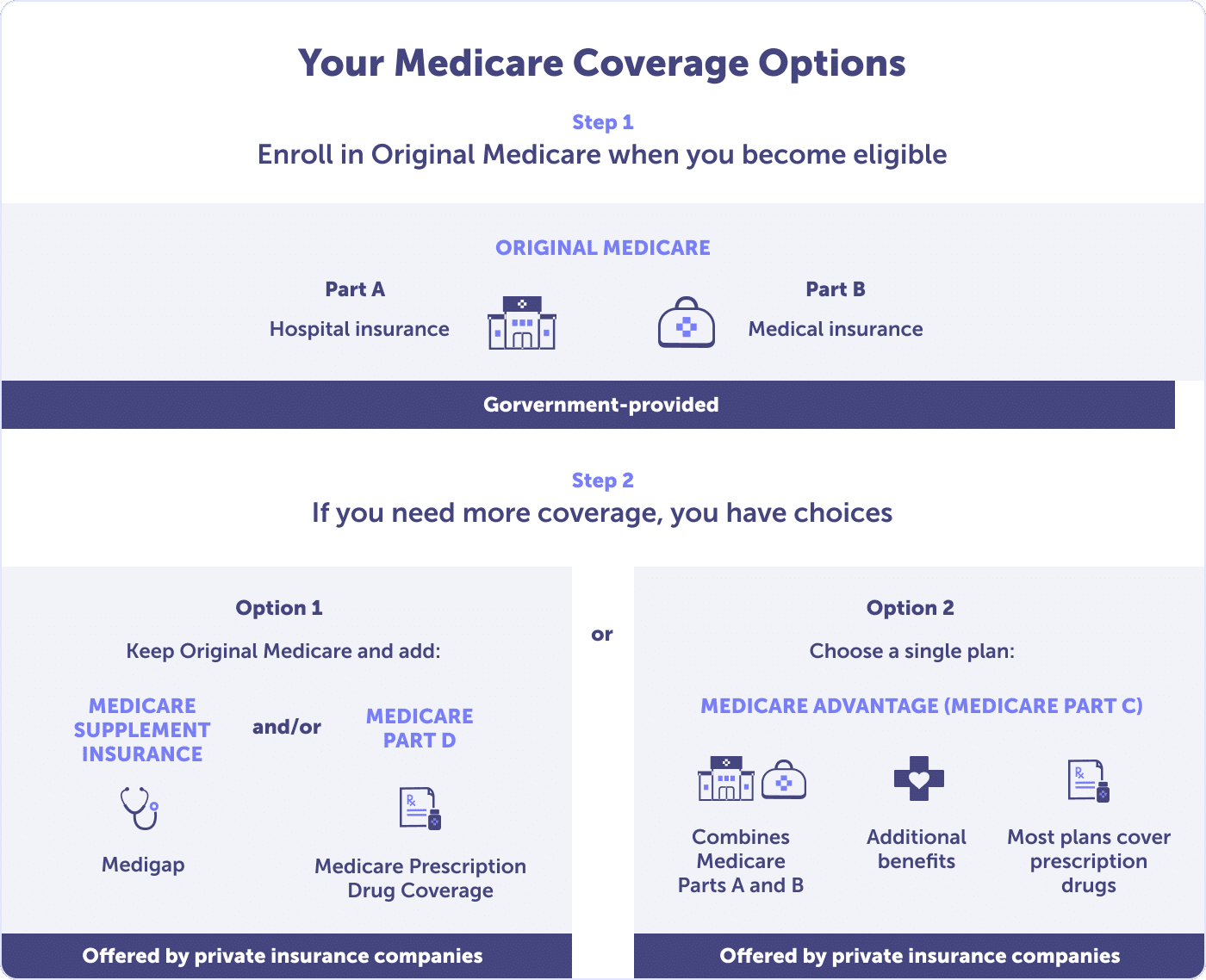
There are several types of plans available under the umbrella of Medicare plans in Arizona, including Original Medicare (Parts A & B), Medicare Advantage (Part C), and Medicare Supplement insurance (Medigap). These plans are a mix of public and private Medicare plan options.
Arizonans have access to the public option provided by the federal government, referred to as Original Medicare. Original Medicare includes Part A (hospital insurance) and Part B (medical insurance). These public plans don’t protect you from high out-of-pocket costs and lack comprehensive dental, hearing, and vision coverage.
Because of these shortcomings, most people enroll in a private health insurance plan approved by Medicare. These private plans include Medicare Part C (Medicare Advantage plans), Medicare Part D (prescription drug coverage), and Medicare Supplement plans (Medigap).
We’ll dive into what each public and private plan option covers so you can find the best combination for your health and budget needs.
Original Medicare Part A (hospital insurance) is a part of Original Medicare and, in most cases, is premium free. Whether it’s premium-free or you must pay, it covers medically-necessary services delivered by a Medicare-assigned healthcare provider – in a Medicare-approved facility.
Part A covers but is not limited to the care you receive in the following settings:
If you choose to enroll in a private Medicare Advantage plan, it must provide the same coverage as Original Medicare Part A.
Agent tip:
“Original Medicare does not have a cap on out-of-pocket expenses which is why most Medicare beneficiaries enroll in a Medicare Advantage or Medicare Supplement plan.“
While Medicare Part A provides hospital insurance, Medicare Part B provides your Original Medicare medical insurance. If you qualify for Medicare Part A, you can also enroll in Medicare Part B. However, Medicare Part B is not premium-free. You should expect to pay a monthly or quarterly premium.
Medicare Part B has a standardized premium for Arizona, as with the rest of the country. The standard premium is based on your or your spouse’s income history. And one or both of your incomes will determine the cost of your Medicare Part B premium. For instance, if you make over a certain amount or your income fluctuates, you may need to pay an Income Related Monthly Adjustment Amount (IRMAA) in addition to the premium.
Your Part B also comes with out-of-pocket expenses. These include an annual deductible and coinsurance. Medicare Part B covers 80% of costs, but you are responsible for 20% of coinsurance. Unfortunately, Original Medicare does not cap its out-of-pocket expenses, which is why most Medicare beneficiaries enroll in either a Medicare Supplement (Medigap) or Medicare Advantage plan.
Your basic medical needs are covered by Medicare Part B. These include, but are not limited to:
As of November 2022, 48% of Arizonans are enrolled in a Medicare Advantage plan. There are 1,428,746 Medicare beneficiaries in Arizona, and 683,738 are enrolled in a Medicare Advantage plan. Medicare Advantage plans, also known as Medicare Part C, provide all the benefits covered by Original Medicare plus additional coverage such as comprehensive dental, vision, hearing, and more.
These plans are offered by private insurers approved by the Centers for Medicare and Medicaid Services (CMS). Medicare Advantage plans typically include prescription drug coverage.
To qualify to enroll in a Medicare Advantage plan in Arizona, you must be enrolled in Original Medicare Parts A and B and live in the plan’s service area.

Original Medicare sets the standard for Medicare coverage. That means that while private insurance companies offer Medicare Advantage plans, they must match the coverage provided by Medicare Part A and B. While Original Medicare does not have a cap on out-of-pocket costs, Medicare Advantage plans do. These plans have set deductibles, coinsurance, and copays within limits established by the federal government.
With a Medicare Advantage plan, you limit out-of-pocket expenses and protect yourself from high and surprise medical bills. Once your Medicare Advantage hits its out-of-pocket limit, including the deductible, the Medicare Advantage plan pays 100% of covered healthcare expenses for the remainder of the year.
Medicare Advantage plans are available on a county level. This means that the plans in one county may not be available in another. In one county alone, there are many plan options to choose from. You will likely have Health Maintenance Organization (HMO), Point of Service (POS), and Preferred Provider Organization (PPO) plan options available to you.
There are 157 Medicare Advantage plans in the state. Between 2022 and 2023, there was a 1.3% change in plan options (155 plans in 2022). Between 2021 and 2022, there was a 29.2% change in plan options (120 plans in 2021).
With 157 plans available, there are numerous options to find the right plan for your health and budget.
Most Medicare Advantage plans include extra benefits that Original Medicare doesn’t offer. These benefits include comprehensive dental, vision, and hearing, plus innovative offerings like wellness and healthcare planning, rewards and incentive programs, and more. Most plans also include prescription drug coverage that you’d need to purchase separately (Part D) if you went with Original Medicare. Medicare Advantage plans that include prescription drug coverage are called Medicare Advantage Prescription Drug plans (MAPD).
Medicare Advantage Prescription Drug plans provide your hospital, medical, and prescription drug coverage through one plan. In 2023, the majority (89%) of Medicare Advantage plans nationally include prescription drug coverage. And, on average, you may have 35 Medicare Advantage Prescription Drug plans.
If you need help or more information about Medicare Advantage plans, Connie Health can help. Call (623) 223-8884 to speak with a local licensed agent.
While you must sign up for Original Medicare Parts A and B, the Centers for Medicare and Medicaid Services (CMS) also requires you have creditable prescription drug coverage. If you don’t have prescription drug coverage, you could face penalties. The source of this coverage could come from Medicare Part D, a Medicare Advantage Prescription Drug plan (MAPD), work, or another source.
Medicare Part D works with Original Medicare Parts A & B. Therefore, if you sign up for a Medicare Advantage plan, you’ll likely get drug coverage through that plan. Part D is provided by private health insurance companies that contract with CMS, similar to Medicare Supplement and Medicare Advantage plans.
Plans are available on the county level, so the cost and availability of a stand-alone Part D plan will vary. There is 28 Part D plans to choose from in 2023. Most plans also require you to pay a monthly premium, annual deductible, copayments, and coinsurance.
There are programs that can help you afford Part D or your prescription medications. Extra Help could provide you with the assistance you need. In fact, 25% of Arizonans enrolled in a stand-alone Medicare Part D plan get Extra Help (Low-income subsidy).
A local licensed Connie Health agent can ensure that your Medicare plan covers the prescriptions you rely upon. If you need help choosing the right plan or seeing if you qualify for Extra Help paying for medications, call (623) 223-8884.
Did you know that you could end up paying penalties if you don’t sign up for a Medicare Part D plan when you turn 65? It’s true. But don’t worry—there are ways to prevent those pesky Part D penalties. Let’s take a look at how to avoid them.
The current penalty system is based on the time since your Initial Enrollment Period (IEP). The IEP is a seven-month window that begins three months before your 65th birthday and ends three months after. If you enroll in a Medicare Part D plan during this period, you won’t be subject to any penalties.
However, if you miss your IEP or decide to wait until later to sign up for a plan, you may be charged a penalty in addition to your plan premium when you eventually sign up for coverage. This penalty is determined by how long it has been since the start of your IEP; for every month without coverage, after your IEP ends, 1% will be added to your monthly premium for as long as you have that plan.
Ensure that you won’t incur late enrollment penalties. Speak with a local licensed Connie Health agent who can review your Initial Enrollment Period and ensure you have prescription drug coverage. Call (623) 223-8884 today.
If you missed your IEP and have now decided it’s time to get coverage, all hope isn’t lost.
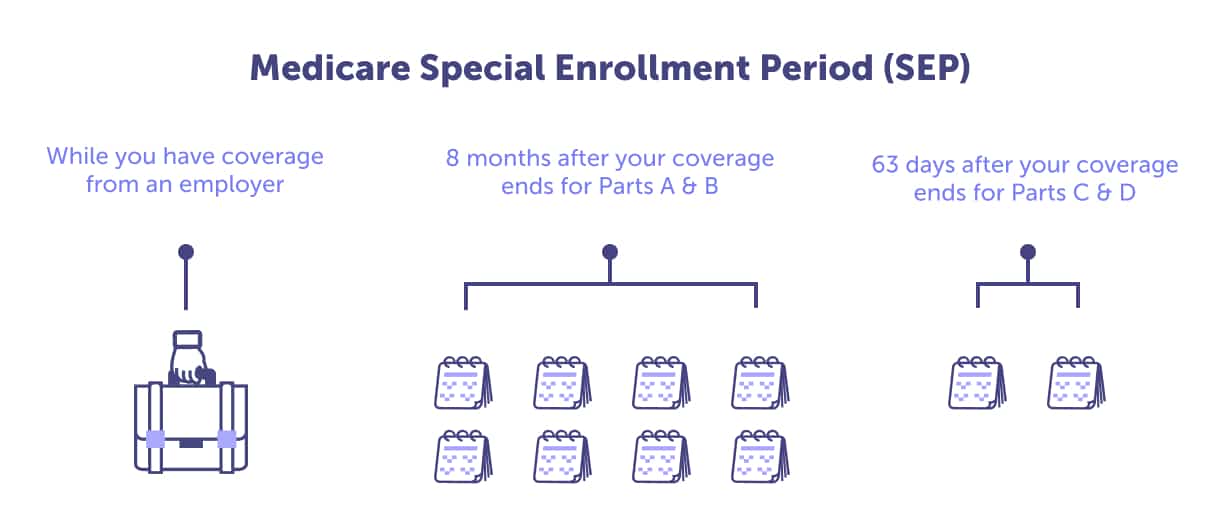
You can still enroll in a Medicare Part D plan through Special Enrollment Periods (SEPs). SEPs allow eligible individuals to join or switch plans outside their IEP window without facing additional penalties due to late enrollment. Some examples of qualifying circumstances include moving outside of the service area of your current plan, qualifying for low-income subsidies, or losing other creditable prescription drug coverage (such as through an employer).
It’s important to note that signing up during a SEP does not waive any existing late enrollment penalties; these will still apply unless they are waived due to extreme circumstances like incarceration or living abroad. However, SEPs allow seniors to avoid any new late enrollment penalties from accruing while they figure out which Medicare Part D plan works best for their needs.
So make sure you take advantage of them. Signing up during a SEP can help ensure you stay covered with quality prescription drug coverage while avoiding costly late enrollment fines and fees.
Original Medicare doesn’t cap its out-of-pocket costs. That’s where a Medicare Supplement can help.
Suppose you’d like to stay on Original Medicare. In that case, a Medicare Supplement (Medigap) plan can help pay for some or all of the out-of-pocket costs, such as copayment, coinsurance, and deductibles. Medicare Supplement plans are sold by private insurance companies approved by CMS but do not include prescription drug coverage.
Because there isn’t a cap on out-of-pocket expenses with Original Medicare, most beneficiaries have additional coverage through a Medicare Supplement or Medicare Advantage plan. Either of these plans can protect you from unknown and surprising medical costs.
A Medicare Supplement plan should be purchased during the Medicare Supplement Open Enrollment Period. If you choose to enroll in this plan type later, you may need to undergo underwriting, which may lead to a more expensive plan premium or plan rejection.
Want to ensure you don’t miss the window to enroll in a Medicare Supplement plan? Call to speak with a local licensed agent at (623) 223-8884. We can help you choose the best plan for your health and budget.
When selecting an Arizona Medicare plan, it is essential to understand your options to make an informed decision based on what best fits your budget and lifestyle needs. There are several types of plans available under the umbrella of Arizona Medicare plans, including Original Medicare (Parts A & B), Medicare Advantage (Part C), and Medigap Insurance policies which help pay for some or all out-of-pocket expenses associated with Original Medicare like copays, coinsurance, and deductibles.
Before making a final decision on an Arizona medicare plan, assess if any additional coverages such as vision care or dental care are needed, as well as take into account any existing medical conditions or prescription medications to ensure that they meet your needs. With these tips, you can make the most of your Medicare coverage.
You may be wondering when the enrollment deadlines are for Medicare. Knowing the deadlines is important so that you don’t miss out on any potential coverage or benefits that may be available. To help, let’s look at the different enrollment deadlines for Medicare in Arizona.
The Initial Enrollment Period (IEP) for Medicare begins three months before your 65th birthday and lasts for three months after your 65th birthday. During this period, seniors must sign up for Part A and Part B of Medicare if they choose to do so. It is important to note that failure to enroll during this period could result in penalties being applied when signing up at a later date.

Not sure when your Initial Enrollment Period is? We’ve created an eligibility quiz that clarifies that question. Enter your birthdate to discover your seven-month Medicare enrollment window.
Not sure if it’s the right time to enroll in Medicare Part A and B? Explore your options with a local licensed agent. Call (623) 223-8884 to speak with an agent today.
If you don’t sign up during your Initial Enrollment Period (IEP), you can still enroll during the General Enrollment Period (GEP). The GEP runs from January 1st to March 31st of every year and is open to anyone who did not sign up during their IEP. If you sign up during this enrollment period will have coverage beginning July 1st of that same year. Note that if you enroll during the General Enrollment Period, it likely means that you missed your IEP and may incur late enrollment penalties.
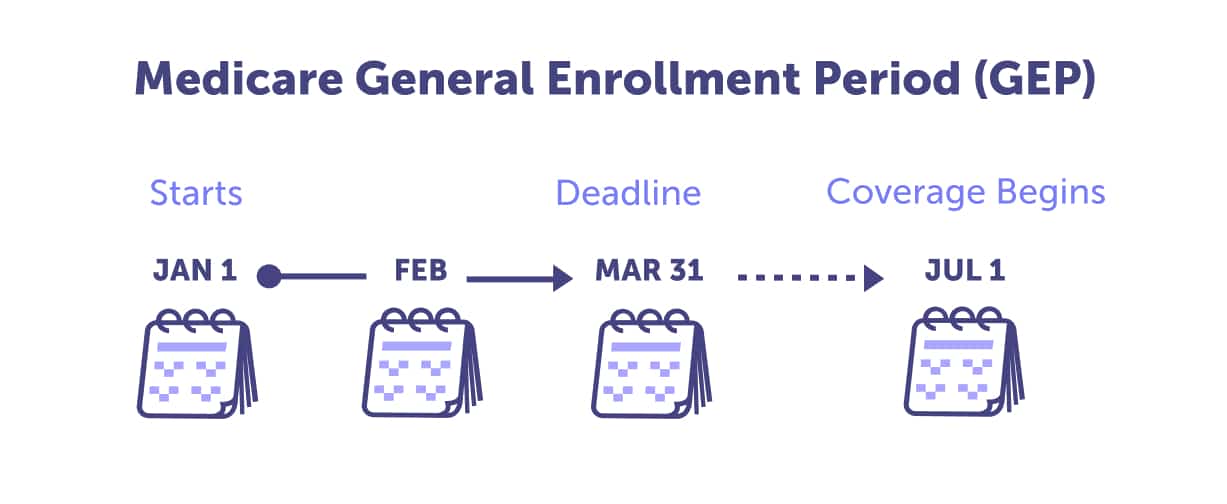
The Initial Enrollment Period and General Enrollment Period are when you’ll most likely enroll in Medicare. However, there are additional enrollment periods that you should be aware of. These allow you to switch to a different plan – often optimizing based on health, budget, or even moving changes. These enrollment periods include:
There may be numerous Arizona Medicare plans for you to choose from. And essential deadlines for you to know. It may seem overwhelming, but Connie Health is here for your entire Medicare journey.
With information about your current doctors, specialists, prescription medications, and extra benefits you’re seeking, a Connie Health agent can find the plan that’s right for your health and budget. Have a local licensed agent guide you through your Medicare journey. Call (623) 223-8884 to speak with an agent today.

Read more by Sammy Menton
I am an Arizona Life and Health Insurance Licensed Agent and have been helping people with Medicare since 2009. I enjoy coaching youth and high school sports, watching sports, and spending time with family. I also like taking road trips and vacationing anywhere that has a beach.